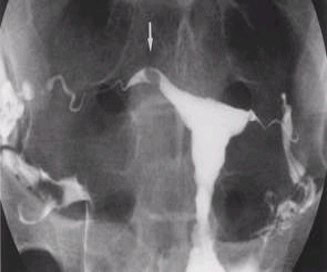
Hysterosalpingogram X-ray
The hysterosalpingogram x-ray is a valuable fertility test used primarily to determine whether fallopian tubes are open. It is both a diagnosis test and a fertility therapy. Pregnancy rates are often doubled or tripled for several months after the HSG x-ray.
What might be found on HSG x-ray ?
Normal uterus and tubes –
The most common result of HSG is normal anatomy. Usually no abnormal uterine or tubal findings are encountered. In this case, the HSG x-ray is still worthwhile due to the significant increase in pregnancy rate for several months afterwards.
Tubes blocked — proximal, mid, or distal
Proximal tubal block is the point where the tube exits the uterus, and blocked fallopian tubes are discovered then a tubal cannulation procedure is done resulting in approximate 70% success in reopening the tube
Mid tubal block – is 2 or 3 inches down the fallopian tube, rarely encountered, cannulation doesn’t work
Distal block — at the end of the fallopian tube, a relatively common finding, can be opened by laparoscopy surgery.
Hydrosalpinx –
A type of distal block where the end of the fallopian tubes fills with fluid and balloons out like a water balloon. This may significantly decrease pregnancy rates as stagnant fluid in the tube cannot escape out the blocked end, so it occasionally backs up into the uterine cavity and poisons embryos. Even In Vitro Fertilization success rates are cut in half or two thirds by the presence of a hydrosalpinx. Cannulation doesn’t work opening this type of tubal blockage. It is fixable by laparoscopy to either open the end of the fallopian tube (neosalpingostomy) or to remove an unfixable tube. After surgery, success rates are typically doubled or tripled.
Salpingitis Isthmica Nodosa (S.I.N.) –
A common type of proximal tubal block, usually opened by cannulation during the procedure.
Filling defects in the uterus
Defects in the uterus are often encountered on HSG x-ray. These tend to be smooth uterine polyps, the most common finding. If they are small and out of the way, no therapy is required and they do not interfere with pregnancy success rates. If they are large or in the middle part of the uterus, they may decrease pregnancy rates, but can be easily removed with a minor 12 to 15 minute outpatient procedure. Other types of uterine defects include small fibroids inside the uterus or scar tissue (Asherman’s syndrome) which is left over from a previous difficult delivery or a dilation and curettage procedure. If minor, it is easily corrected and does not interfere with subsequent success rates. If a significant amount of scar tissue is present, then a more advanced hysteroscope correction procedure will be required, but usually results in good pregnancy rates afterward.
Uterine anomalies
These include congenital uterine defects such as uterine septum, didelphic uterus, T-shaped uterine cavity, or asymmetrical uterine cavity. These defects, including T-shaped cavity, are usually correctable by operative hysteroscopy procedures.